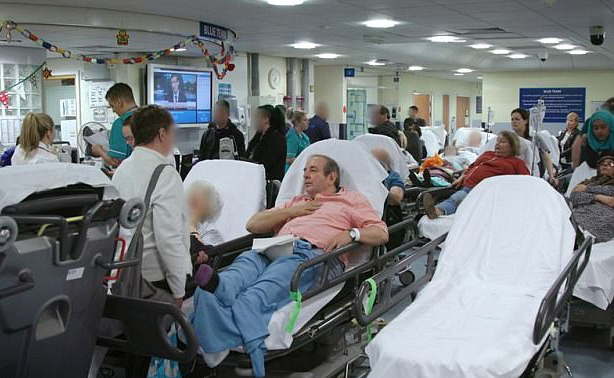
Is the winter crisis a new phenomenon?
A winter crisis in the NHS may not be an entirely new phenomenon, but the severity of it is. 2012-13 saw the first reports of a winter crisis, but the situation has deteriorated dramatically since then as funding has not kept pace with the added demands placed on the service, while a collapsed social care system leans on the NHS very heavily. As we have previously reported, since 2010 the NHS and social care have been significantly underfunded and we are increasingly witnessing the amassed effects of government mismanagement.
In 2016-17 winter pressures and a cumulative lack of funding combined in dramatic fashion. The Red Cross notoriously declared “a humanitarian crisis” after witnessing the conditions both patients and staff were forced to endure. Comparing the working environment of a healthcare system in the 6th richest world economy to a war zone is a new feature of the standard ‘winter pressures’, and it is in serious danger of being normalised. This year the press are ready and expecting the worst. In the first four days of 2018, there were more mentions of “NHS” with “winter crisis” in British newspapers than in the entire period from 2003 to 2009.
The truth is the NHS is suffering a ‘crisis’ all year round which is merely exacerbated during the winter months. There is no slack in the system so when there is an increase in demand it struggles to cope. The word crisis implies an unforeseen and dramatic event; yet conditions during the winter should be neither of these. All it does is lay bare the inadequacies of the system year-round. Contingency should be made to deal with the major issues that create unmanageable situations instead of simply pretending they have come out of nowhere, there was nothing that could have been done, or worse still – as has happened in the past – denying there is even a problem at all.
What has the government done about it?
Last year saw the worst winter conditions in over 10 years, and this year will be even worse. This year the government has spent a total of £181.3m in preparing for winter and £240m on adult social care to try and minimise the issues in discharging patients. However, this offering falls far short of what is needed. It equates to only £1.6m when divided equally between all local authorities, and crucially is not ringfenced so in all probability will be utilised for other demands. Last year £337m was injected into the system, but it was too little, too late and consequently had almost no effect in mitigating the crisis in hospitals.
Latest figures from NHS England
The latest figures from NHS England released last week as part of their annual weekly winter reporting make for some unsettling reading. Figures show that this winter is already worse than 2017. Last month the target of 95% for seeing and treating patients within the 4-hour window slipped to 87.6%, the lowest ever on record for a November.
In addition, last month saw nearly 55,000 patients spending over four hours on a trolley waiting for a hospital bed, with 258 of them waiting for at least 12 hours. A total of 54,631 patients waited more than four hours for an inpatient bed in November, 12% higher than last year. In comparison, 48,730 patients had to wait in busy A&E departments last November – nearly 11% fewer. The NHS is now recruiting corridor nurses as standard practice which in itself should shame this government into action, but so far this doesn’t seem to have registered as an issue.
It is important in all of this to not lose sight of the fact that there are people behind these numbers. There are lives put at risk unnecessarily, and for each statistic there are countless heroic efforts of staff members which stop the figures being higher still. These are the people who struggle daily for very little reward, and who are regularly put in dangerous situations just to keep the NHS functioning.
Fully occupied
Around the country 94.2% of beds were occupied in the first week of this month and 1 in 10 hospitals had no free bed on at least one night in the first week of December. Figures from NHS England revealed that in the first week of this month 14 out of 134 hospital trusts spent at least one night with all of their beds occupied and being at minus beds, although vastly unsafe; is not uncommon.
Staff in our NHS are braced for impact. Despite these figures it is important to remember that neither seasonal flu nor bad weather has yet hit to any great degree. With the lack of contingency, the effect of a particularly bad bout of either is now a very worrying prospect.
Ambulance waits
So far this winter 10,675 (1 in 9) patients have spent at least 30 minutes waiting with ambulance crews before A&E staff took over and 1,939 – one in 50 – waited outside the A&E for more than an hour. This practice clearly puts lives at risk, not to mention breaking NHS guidance. Ambulances were turned away from hospitals 25 times in the last week and sent to nearby units due to a lack of capacity.
Not only do these delays risk the safety of those waiting to be seen, but it also means there are fewer emergency vehicles to be dispatched, and that staff are almost certainly working more than their allotted hours. The overall effects of delaying ambulances are very difficult to quantify, but the pattern already emerging this winter is deeply concerning.
Trusts in debt
Added to this, the NHS is still struggling to cope with the debt incurred from last year’s winter crisis. The cost of breaching targets, (not to mention cancelling operations), has hit trusts hard. The fine is £120 for each breach of the 4-hour A&E target which mounts up significantly during winter. The cost of cancelling 50,000 operations last year alone was estimated by the government to be around £68m, which incidentally equates to the cost of employing 15,000 nurses. At a meeting of the committee of public accounts this week the department of health and social care refused to rule out the same scenario happening again. This behaviour is symptomatic of the government’s attitude towards public services generally and their apparent ideology of running them down in order to create fertile ground for privatisation.
Average theatre costs per hour also vary substantially, and there are no official estimates. NHS Providers has put this at £561p/h, while in 2009 the NHS Institute for Innovation and Improvement (now closed) said this could be as much as £1,200p/h. That would suggest somewhere in the range of £193m-£413m could be being lost every year as a result of the impact of shortages on planned surgeries alone.
Financially penalising individual trusts for circumstances beyond their control makes no logical sense and only serves to exacerbate an already impossible situation. Robbing Peter to pay Paul then becomes the only viable solution so other areas of care inevitably suffer. Trusts are being set up to fail by a government who cannot or will not properly fund and manage an event that happens every year.
In October this year there have been 405 cancellations of urgent operations, 42% over the figure of 287 for October 2017. It is folly for NHS England to impose targets and fines when it is obvious they cannot be reached. The government is setting the NHS up to fail in every conceivable way.
A crisis all year round?
In October 2010 when the Conservative-led coalition government came to power, 6,932 patients waited more than 3 hours in A&E. By October 2017 that figure had risen to 45,532. This dramatic growth illustrates how dire the situation has become and just what happens when 15,000 hospital beds are cut. It shows how an underfunded and understaffed system cannot possibly keep pace with demand. And yet, despite the unprecedented demand for hospital beds and the extreme pressure put on the health service, in September 2017 there were 82 wards closed and 1429 beds were empty because the NHS did not have the funding or the staff to keep them open. That the government can leave the NHS in such dire straits but seemingly find money for other policies (such as promoting unproven app-based medicine) when it deems it necessary, is unacceptable and unsafe.
Winter or not, there are nevertheless over 100,000 NHS vacancies and no sign of a solution. How long will it be before summer sees just as widespread a crisis? How long before the situation in UK hospitals causes the service to collapse completely? We need a change of government, or a dramatic shift from this one in imposing damaging financial penalties upon trusts. The government needs to utilise resources properly in combination with increased and sustained year-round funding in order to alleviate (and next winter to stop) scenes that are now sadly all too common.
Samantha Wathen, Press and Media Officer for Keep Our NHS Public

Leave a Reply