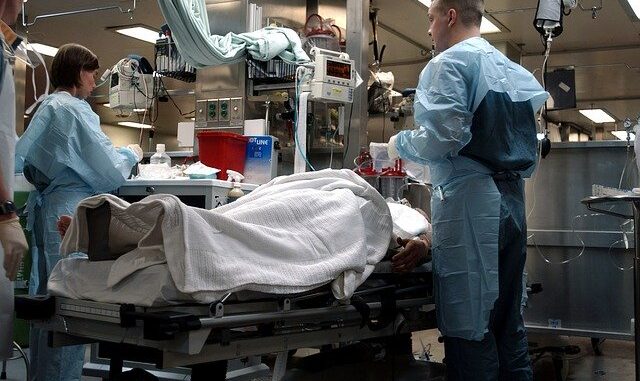
It has been a long time since the NHS was properly staffed, since people went home on time, or had manageable workloads. It’s been several years since winters were workable. The months from October to March have been referred to so often as a ‘winter crisis’ that the words have largely lost all meaning, It’s been too long since lines of queuing ambulances outside hospitals were not a permanent feature of winter up and down the country.
Staff have been forced to adapt to potentially dangerous rota gaps being the norm, or bed capacity being routinely breached. Expensive private agencies are now routinely relied upon to plug unsafe staffing gaps, and NHS staff at all levels feel both undervalued in their work, and endlessly put upon by a system in a state of perpetual emergency.
The NHS has barely enough staff to cope in normal times. The vacancy rate now stands at over 100,000 and this is predicted to rise significantly as highly demoralised staff decide enough is enough and vote with their feet.
A survey conducted in July by the Royal College of Nursing shows that the percentage of nurses thinking of leaving the profession has increased to 36%. Of those 61% cited pay as a factor, with other factors including the way nursing staff have been treated during the Covid-19 pandemic (44%), low staffing levels (43%), and lack of management support (42%).
The government consistently refuses to address the root cause of this gaping hole in the workforce – namely better funding for the health service which makes it an attractive place in which to work. Increasing funding to the necessary levels would create capacity in the system, more beds and equipment, better IT infrastructure, research opportunities and career development. A decent living wage would encourage people to come back into the NHS, and make them feel genuinely valued. Rather than looking at root causes for this alarming level of dissatisfaction and seeking to address them, this government has now even stopped the brief respite from parking fees for staff and left the majority of healthcare workers out of a public sector pay increase.
At the beginning of the first wave of Covid-19, seven temporary Nightingale hospitals were set up to manage the predicted overspill of COVID patients when established hospital beds reached capacity. There has been much talk about the ingenuity behind these temporary facilities - and admittedly the making possible of these units is to be commended. However, the need for the existence of these urgently-created hospitals is a powerful illustration of how little wriggle-room exists in our hospital system and how resilience has been stripped away by chronic underfunding.
What is not mentioned by the Government, in their self-congratulatory celebration of rapid engineering, is exactly who will staff these temporary hospitals. Dozens of patients with Covid-19 were turned away from the Nightingale hospital in London during the first wave of infection because it had too few nurses to treat them; and this was when the ITUs were at full stretch and the vast majority of routine NHS elective work had been cancelled to free-up capacity in the system.
The beds in Nightingale hospitals total up to 11,500 and this time round, even more than in April, there will be no option but to try to poach staff from established hospitals to operate them, because elective services have so far been told to continue running a ‘normal’ NHS. In the spring, staff were redeployed from non-urgent specialties to work across acute care. Now trusts in England face fines for waiting lists caused by the necessary cancelling of non-COVID work.
This ‘robbing Peter to pay Paul’ strategy has obvious pitfalls, leading many in the NHS to view this essentially as not much more than a government PR exercise. Estephanie Dunn, regional director of the Royal College of Nursing in the North West said:
When the Nightingales were originally introduced in the first wave of the disease, airline cabin crew who were not being utilised in their jobs were asked to join NHS staff in running the field hospitals. But, as admirable as this work was, there is a stark lack of clinically trained staff needed to manage a further peak of this pandemic.
Now we are into the second (wholly avoidable) wave, Health secretary Matt Hancock tweeted last week that Nightingale hospitals in Harrogate, Manchester and Sunderland were on standby, adding; “Let’s get COVID under control and save lives.” However, far from being in control of anything, needing to re-open emergency field hospitals isn’t a sign the government are taking control, but more a sign that all control has been lost.
In reality, with the virus increasingly spiralling out of control and no effective measures yet introduced, there is the potential that the Nightingale hospitals will be needed much more than they were in the first wave. NHS staff will be spread even more thinly, putting their mental health and wellbeing at risk, creating further workforce gaps and ultimately threatening the safety of patients and staff alike.
This pandemic has provided fertile ground for the Government to plough ahead in earnest with the rapid acceleration of the private sector in UK healthcare. Billions of pounds of taxpayers’ money are being paid to private companies to clear waiting list backlogs accumulated due to a decade of underfunding. The private sector should have been requisitioned into national service – but now it stands to massively benefit. This situation will only escalate when yet more demoralised NHS staff leave the service, and private companies swoop in to pick up the pieces.
At some point the Government must concede that, due to their historic neglect of the NHS, stopping elective and non-urgent work - as was done during the last peak - is sadly the only way to stand a fighting chance against what’s now coming. When the dust has settled, they face the reckoning that it was their collective ineptitude, grotesquely misplaced priorities and obsession with throwing money at private companies that put the health of all of us at dangerous risk.
Samantha Wathen is the Press Officer for Keep Our NHS Public






Leave a Reply