January 23rd 2021 marks the first anniversary of the Wuhan lockdown and is ten months from when the UK first introduced restrictions on people’s movement in order to decrease the spread of the virus. In this brief overview, I want to look at where we are now and what the Westminster government has or has not learnt.
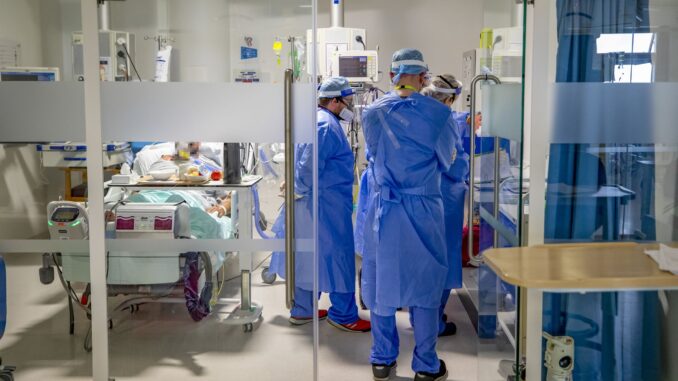
On January 1st this year we recorded a record peak of 69,000 new cases of COVID-19 in one day. The Whittington Hospital in North London currently has 66% of its beds occupied by patients with COVID-19, and is one of 11 trusts with over 50% beds occupied by this disease. There are 32,000 infected hospital inpatients, a figure 70% more than in the first peak. 4,600 patients are receiving critical care, 75% of whom are less than 70 years of age indicating that it is not just the very elderly who are becoming sick.
Huge pressure is being put on NHS staff and absence levels from a combination of sickness and contact self-isolation is around 14%. There is an enormous amount of psychological stress being caused by current working conditions and through not being able to deliver best quality care. This will take its toll on the mental health of care workers for years to come.
The government still claims to be leading the fight against COVID-19 and to have done everything correctly and at the right time – yet after 10 months of fighting the pandemic, how can we still be in this situation with a death toll in proportion to population even higher than that resulting from the chaotic situation in the United States?
How did we get here?
There has been a deadly kind of groupthink from the beginning, apparently shared by conservative politicians and senior medical advisors. What ever was happening in some distant place called Wuhan could not possibly come to trouble these shores –its no worse than ‘flu – we will soon get herd immunity – “let the virus move through the community and we’ll take it on the chin”. Even the deputy Chief Medical Officer claimed that our preparedness for a pandemic was an exemplar to the world. The reality was that recommendations from recent government pandemic planning exercises had been disregarded – the state took out third party rather than fully comprehensive insurance because it was a lot cheaper, and messages from China about the seriousness of SARS-CoV-2 were ignored.
The NHS, underfunded and understaffed, was not in a good state at the start, and it has neither been protected nor has it coped. What the government means by ‘coping’ is that so far, there have been no pictures in the press of people seen to be dying because of lack of intensive care – this is their nightmare, and it may still come to pass. However, to maintain intensive care capacity many services were stopped. This had a huge knock on effect on non-covid conditions. For example, it is estimated that there will be an additional 18,000 cancer deaths from delayed investigation and treatment.
The government must stop blaming others and take responsibility
At the very outset, the suggestion of probable public non-compliance was flagged up in the dubious guise of ‘behavioural fatigue’, used to justify delay in initiating lockdown in March and at other times since then. Public health messaging was terrible, with many interpreting the handling of the Dominic Cummings affair as one rule for the elite and another for the rest of us. Going to the pub became a “patriotic duty” but was later blamed for an increase in cases, as was the “eat out to spread the virus” scheme. Dangerous family mixing for five days over Christmas was encouraged, and then reduced to one day at the last minute. Against the advice of the teaching profession schools were declared safe, only to be closed on the day that children went back. The influence of lockdown sceptics on government policy can be seen time and time again.
Meanwhile, the government has been blaming anyone but itself. Over seven hundred health and care workers have died, with those who have been infected often blamed by managers for not following official guidance. Shortages of Personal Protective Equipment (PPE) were first denied and then blamed on workers using PPE inappropriately. Public Health England (PHE) was blamed for not providing tests despite this not being one of its roles and PHE laboratories having been abolished. In any case, following the 2012 reorganisation PHE was not an independent organisation but under the management control of the Health Secretary, so that any of its failures are his failures. To abolish PHE in the midst of the pandemic was described as “taking the wings off a malfunctioning aeroplane while in flight in order to ensure a safe landing”, an analogy that highlights the government’s rash and ill-judged reactions to events.
The second tsunami
Now we have a virus mutation blamed for escalating case numbers, despite the evidence that these were going up in December before its appearance and when Tier 4 restrictions were clearly not working. Mutations arise because of rapid spread of infections - in other words as a consequence of loss of infection control rather than a cause – less infection, less chance of a mutation.
The government was warned in September 2020 that major change in response was needed to prevent a surge in cases but, as always, was disastrously slow to respond. It has pursued a short term strategy of suppressing the virus and hoping for an effective antiviral treatment or vaccination to come along, searching in vain for a magic bullet rather than setting in place a raft of measures under the guidance of public health experts.
The current figure for deaths in the UK from COVID-19 is 110,000, but this is likely to be an underestimate. Data from a Leicester study is showing that 30% of covid-19 patients discharged from hospital are readmitted within 5 months and 1 in 8 of these die – missed from the ‘death within 28 days’ definition.
Vaccination dividend
The prime minister is no doubt desperately wanting to take the credit for an effective vaccination programme in the hope that criminal incompetence will be forgotten. The rapid development of effective vaccines is a major positive development and a scientific triumph, but the £350 million contract that has been given to Lord Ashcroft’s (a former party chairman and major donor) company is another example of the outrageous cronyism that has been all to evident and should be no part of a response to a pandemic.
Let us also remember that official guidance is preventing people without an NHS number getting vaccinated and this includes not just undocumented migrants but some NHS and care workers from overseas – an absolutely disgusting situation. As roll out of the vaccine continues at pace, we should remember that this is down to the efforts by staff of a National Health Service. All credit for a successful outcome should be given to a publicly funded, publicly delivered health system and be used as an argument for future investment.
It really could have been so different
There are places like New Zealand, Hong Kong, Taiwan and South Korea that pursued an elimination strategy aiming to exclude disease and eliminate community transmission. This greatly reduced cases, protected health services, saved lives, and averted serious health inequalities. Their economies were actually protected, performing more favourably than countries like the UK that pursued a suppression strategy. In New Zealand there have been just 25 deaths; if we had replicated this approach it could have been translated into 340 deaths in the UK, not 110,000.
Shaming and blaming
Rather than look to its own failures the government much prefers to blame the pubic for not obeying rules, talking of ‘flouting’ or ‘brazen defiance’ by the population at large and using the flawed concept of pandemic fatigue as an explanation. The impression is reinforced by media attention focussed on examples of rule breaking such as house parties, involving only a tiny fraction of society. The problem is presented not as government failing to meet its responsibilities but widespread non-adherence to rules – a function of poor psychological motivation, more prevalent in certain communities.
The reality is quite different, with repeated surveys showing a very high proportion of the population (over 90%) observing behavioural regulations. According to Office of National Statistics, even much demonised students in reality showed a very high level of social distancing and low levels of mixing.
The main area of non-compliance is for self isolation if infected or a contact – only around 18%. Why is this? - because self isolation requires support that is still not available. Contrast with New York where money, accommodation, counselling, food and even pet care were provided and compliance was 95%.
The bottom line is that people get infected because they get exposed. This happens if you are poor, live in crowded housing, cant (or are not allowed) to work from home, and are dependent on public transport. The costs of an obsession with getting people back into crowded work places has been highlighted with the 500 cases among staff of the government Driver and Vehicle Licensing Agency’s offices in Swansea.
Judgement is coming
The narrative of blame conveniently projects real government failures onto imagined failure by the public. Despite the vaccination programme we must insist that the government is judged on its record - over 110,000 deaths – the worst death rate in the world – and still rising. Vaccination is not the elusive magic bullet and, like mass testing, like the app, like the tiers – will not bring us quickly back to a pre-covid normality.
We still need an elimination/Zero Covid strategy, a comprehensive ‘find, test, trace, isolate and support’ system based in local public health teams – and these things still need to be implemented urgently to prevent even more wasted lives.
Keep Our NHS Public will be reviewing all of these issues in its soon to be launched ‘People’s Inquiry into Covid’. The main lesson will be that it has been political choices that have got us where we are and a changed political landscape is needed if we are going to implement the ‘Rescue plan for the NHS’ and build the kind of publicly funded, provided and accountable health service that is so desperately needed.
Keep Our NHS Public co-chair Dr John Puntis







I have mail from my MP stating categorically that the NHS IS NOT AND NEVER WILL BE, in part or as a whole for sale. What am I to make of this please?
We might have fewer deaths if our testing were better. PCR tests and gene testing are fine but Lateral Flow Tests- rapid tests are not. They may miss positives in asymptomatic people and in so doing help the spread of the virus. The inaccuracy of these tests has been known since last October: https://www.bmj.com/content/371/bmj.m4950
There are better, rapid tests available, but scientists and the government seem to have turned a blind eye. Dominic Cummings said that we would “get ahead of the science” with LFT. This may be costing lives.