
The latest NHS staff survey published earlier this week reveals the effects of an underfunded and understaffed system on those who work in it, and highlights how their health and wellbeing is at risk
The NHS Staff Survey has been conducted annually since 2003 and is one of the largest in the world, open to 1.1 million people. This year nearly half a million staff (497,117) across 230 hospital trusts participated
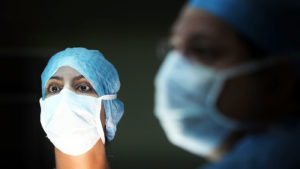 The response has been damning. According to the British Medical Association (BMA), the latest survey shows that the service’s workforce is ‘in crisis’. Denis Campbell, Health policy editor for The Guardian, wrote in his piece, NHS England survey reveals 'alarming downturn' in staff wellbeing,
The response has been damning. According to the British Medical Association (BMA), the latest survey shows that the service’s workforce is ‘in crisis’. Denis Campbell, Health policy editor for The Guardian, wrote in his piece, NHS England survey reveals 'alarming downturn' in staff wellbeing,
Poor morale could exacerbate the already serious understaffing in the NHS, which has more than 100,000 unfilled vacancies – one in 11 of all posts. The survey found 51% of staff were considering leaving, 30% often thought about leaving the trust they worked for, 22% planned to look for a new job with a different trust in the next year and 16% intended to leave as soon as they could find another job.
All of this is of course has been predicted by Keep Our NHS Public on many occasions, see here and here.
The Findings
The key findings of the survey include:
- A majority (51%) are thinking about leaving their current role and 21% want to quit the NHS altogether.
- More than three-quarters (78%) feel under unrealistic time pressures some or all of the time.
- Nearly six in 10 (58%) say they do unpaid overtime every week, though that number is falling.
- Nearly 28% have suffered back pain in the last year as a direct result of their work, up two percentage points since 2017.
- Fewer than three in 10 (28.6%) feel their trust takes positive action to improve staff health and wellbeing.
While this won't surprise campaigners, who will rightly feel vindicated by these findings, it must however shock the general public and those in power, into action.
Only 28.6% felt their organisation takes positive action on health and wellbeing (down 3% on the year before). Overall there is a continuing decline in the health and wellbeing of staff. This trend was consistently observed across all trust types. Ambulance trusts were scored separately, but their figure was lower still at just 22.5%.
Last week health secretary Matt Hancock outlined a very welcome 90-page document on ‘caring for the carers’, in which he proposed decent on-site facilities for staff to rest in and a programme to support the mental health of the workforce. None of the proposals are revolutionary however and they should already be in place. These proposals must not remain words on a page, and must be given the funding and resource they need in order to be effective. In April the recommendations of this report will go through the final process to see which parts will be formally adopted.
Due to unprecedented staffing pressures, there is a significant onus on workers to attend regardless of their own ill health. 56.5% of those surveyed had gone to work despite not feeling well enough to perform their duties in the last 3 months, while 39.8% reported feeling unwell as a result of work-related stress in the last 12 months. This figure has been rising since 2016 with this being the worst in 5 years.
Unsurprisingly only 22.2% of workers said they never or rarely have to deal with unrealistic time pressures. Sustaining a job in which every day is a struggle due to a lack of beds, resources and staff takes its toll and, in many cases, will eventually lead to ill health and absence from work. Working flat out on long shifts, often without proper breaks is both unacceptable and unsustainable. However, the 10-year plan which has been so hailed as a solution to NHS pressures contains no workforce plan and there is no solution yet being offered to this now normalised way of working.

Staff do not feel valued
The NHS employs some of the most talented people in the world. However, less than half of those responding (46.1%) said they were satisfied with the extent their organisation values their work.
Non-mandatory training has seen a continued decline with this year’s results being the worst in 4 years. There is neither the time nor the resource to devote to non-essential professional development in an understaffed and underfunded system.
NHS workers deserve better.
Not safe, not fair
Out of 309 workplaces, 89 reported a significant increase in the percentage of staff witnessing potentially harmful errors, near misses or incidents in the last month. This figure (of 27.8%) is up 3% from the year before.
With a clinical vacancy rate of over 50,000 it is unsurprising that these incidences are on the increase. The problems in the NHS should not only concern those who work in it. They affect staff and patients differently but are equally concerning to both.
Only just over half of those surveyed (58.2%) said their organisation treats people involved in an error, near miss or incident fairly. Staff need to be assured that if they make an error they will be treated fairly and not scapegoated for government mismanagement, which has sadly happened in the past.
Running on goodwill
It is no secret that the NHS runs on the goodwill of its staff putting in extra (often unpaid) hours in order to keep things running smoothly and provide the best patient care. However, the frequency with which this is happening places NHS staff in an unfair and frequently unsafe position. Close to 3 in 5 (57.8%) are now working unpaid hours every single week, and with predicted staffing forecasts this figure will climb higher still. It is not surprising therefore that over half those questioned (51.1%) were considering leaving and 23.2% wanted to leave the NHS altogether.

To save the NHS, we must campaign against this Governments programme of privatisation and cuts but also properly value its staff. The results of this survey should provide a wake-up call to this government, whether Hancock's 'Caring for Carers' paper will amount to much is yet to be seen, judging by the Conservative Government's track record it looks unlikely. Ministers must commit to addressing the root causes of dissatisfaction and stress at work. Clinicians are exhausted and stressed from endlessly covering rota gaps, many live with the constant worry of making errors in a depleted system and are consequently disenchanted with practicing medicine.
This squandering of talent is a tragedy both on an individual level and for the NHS as a whole. The NHS must employ more staff to address the root causes of dissatisfaction and make it once again an attractive place in which to work. The health service must be properly funded to avoid next year’s survey yielding even more damming results. Amidst a culture of putting up and shutting up, where in many instances speaking out is contractually constrained; this survey is the only way staff in our NHS have of letting us hear their voices – and the Government needs to listen.
Samantha Wathen,
Press and Media Officer
Keep Our NHS Public






Leave a Reply